I’m writing this blog series on Women’s Health to shine some light on some of the topics that you might not be aware of, or just feeling afraid to start the conversation. Fortunately, it is an area that physiotherapists are trained for. So, don’t suffer in silence anymore.
In this first blog, I’d like to tell you first about what is Women’s Health Physiotherapy. It is a physiotherapy area that covers a wide range of issues that can affect women of all ages. That includes issues related to the pelvic and reproductive organs, sexual health, pregnancy, childbirth, and pelvic pain.
One of the most common women’s health issues is stress urinary incontinence / leakage. It is a very uncomfortable and inconvenient issue. Did you know that at least one third of women (and men) suffer from urinary incontinence (Australia Institute of Health and Welfare, 2013)? So, it’s about time we understand what is actually happening when you’re experiencing this problem. Check out the diagram below. The closure of the urethra is mainly controlled by your external urethral sphincter muscle and pelvic floor (PF) muscle. Both of them work together to close the urethra to prevent leaking. However, when the pressure provided by those muscles is overpowered by the pressure of the bladder, leakages can occur. This may happen when you are coughing, sneezing, lifting heavy weights, or jumping. So, strengthening your PF muscle must be your top priority. Keep an eye out for my next blog, ladies! I will be explaining how to activate and strengthen it.
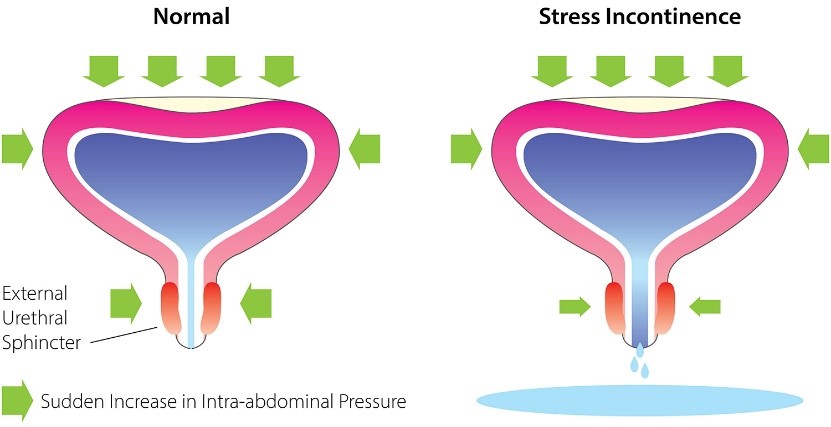
Figure 1. https://urolon.com/urolon-for-women/stress-urinary-incontinence/
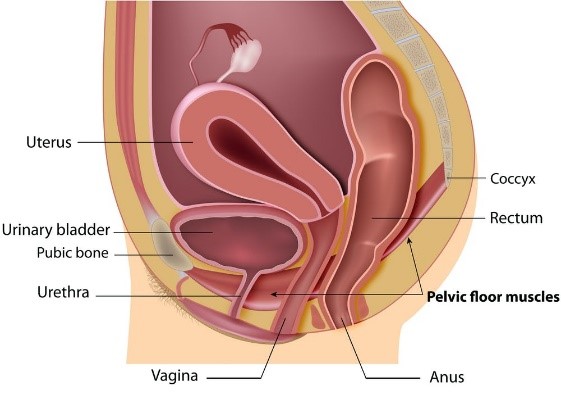
Figure 2. https://theconversation.com/urinary-incontinence-can-be-a-problem-for-women-of-all-ages-but-there-is-a-cure-49365
Another common PF related issue is pelvic organ prolapse. That is when your uterus, bladder, or rectum is slipping down due to weakness/sagging of your PF. The diagram below will show you what it is about. The management of pelvic organ prolapse is mainly prevention. Strengthening your PF muscle should be your first strategy. Other procedures can be done to slow the progress of prolapse. That includes using a pessary device, putting in place a mesh or other surgery repairs.
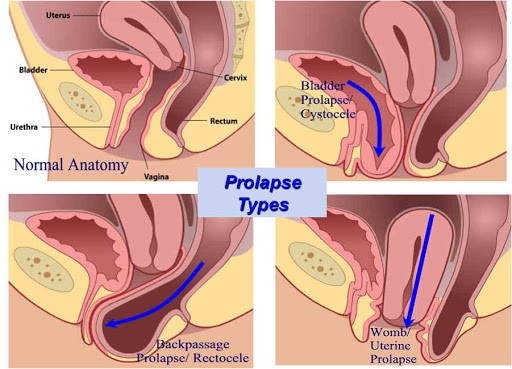
Figure 3. http://petersphotogallery.com/vanea/pelvic-organ-prolapse-pop/
Last condition that I would like to discuss is Rectus Diastasis (abdominal separation) that results from pregnancy. Quite often in the clinic, I hear pregnant ladies worrying about this. The statistics do justify this, as 39% of the women in a study experienced separation even at 6 months post-childbirth (Mota, P, et al, 2015). As you get further into your pregnancy, your rectus abdominus (“six packs”) muscle will stretch out at the linea alba (check out the diagram below). So, as a general rule, sit ups during pregnancy should be avoided to prevent or reduce severity of separation. Instead, you should focus on activating and strengthening your Transverse Abdominis (TA / corset) muscle in order to stabilise and provide support for your pelvis and spine. So brace your core, ladies! The good news is when you activate your PF muscles, your TA muscle will automatically activate, as well (Arab A, et al, 2011)! 2 birds, 1 stone…

Figure 4. https://warriortechocr.com/2018/07/17/diastasis/
I certainly hope you find this blog helpful if you have or know anyone with any of these issues. As I have mentioned above, I’d like to start the conversation among us regarding women’s health. Many out there are suffering in silence, and you don’t have to be. Many of the issues are preventable, and treatable. Don’t leave it too late! In part 2 of the blog series I will be talking more about PF exercises. So, keep your eyes peeled. If you have any concerns, issues, or questions, be sure to contact us.
References:
Australian Institute of Health and Welfare 2013. Incontinence in Australia. Cat. no. DIS 61. Canberra: AIHW.
Arab, A., Chehrehrazi, M., & Arab, A. (2011). The response of the abdominal muscles to pelvic floor muscle contraction in women with and without stress urinary incontinence using ultrasound imaging. Neurourology and Urodynamics, 30(1), 117–120. https://onlinelibrary.wiley.com/doi/10.1002/nau.20959
Mota, P., Pascoal, A., Carita, A., & Bø, K. (2015). Prevalence and risk factors of diastasis recti abdominis from late pregnancy to 6 months postpartum, and relationship with lumbo-pelvic pain. Manual Therapy, 20(1), 200–205. https://doi.org/10.1016/j.math.2014.09.002
